California Gun Stores Win: Court Rules Pandemic Restrictions Violated Rights
Federal appeals court rules two California counties violated rights with pandemic gun store shutdowns, throwing a wrench into the complex relationship between public health measures and constitutional rights. The ruling, a landmark decision, found that the counties’ restrictions on gun store operations during the pandemic violated the Second Amendment rights of gun owners.
This decision has sparked a heated debate about the balance between public health concerns and individual liberties during emergencies.
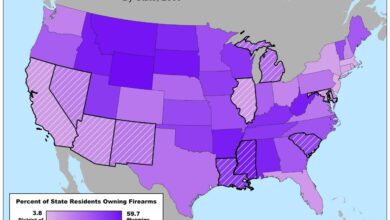
The case stemmed from the California counties’ decision to classify gun stores as non-essential businesses during the early days of the pandemic. This designation forced gun stores to close their doors, effectively restricting access to firearms for many residents. Gun store owners argued that the restrictions were arbitrary and disproportionate, violating their right to sell firearms and the right of citizens to purchase them.
The court ultimately agreed, finding that the restrictions were not sufficiently tailored to address the pandemic’s threat and unduly burdened the exercise of Second Amendment rights.
Second Amendment Rights: Federal Appeals Court Rules Two California Counties Violated Rights With Pandemic Gun Store Shutdowns

The Second Amendment of the United States Constitution guarantees the right of individuals to keep and bear arms. This right is not absolute, however, and has been subject to various interpretations and legal challenges over the years. The recent ruling by the federal appeals court regarding California counties’ pandemic-related gun store closures brings the Second Amendment’s application in contemporary contexts into sharp focus.
Supreme Court Interpretations of the Second Amendment, Federal appeals court rules two california counties violated rights with pandemic gun store shutdowns
The Supreme Court has played a significant role in shaping the understanding of the Second Amendment. In the landmark caseDistrict of Columbia v. Heller* (2008), the Court ruled that the Second Amendment protects an individual’s right to possess a firearm unconnected with service in a militia, and to use that arm for traditionally lawful purposes, such as self-defense within the home.
This decision overturned a century-old precedent that had interpreted the Second Amendment as applying only to the collective right of states to maintain militias.The Court further clarified its interpretation inMcDonald v. City of Chicago* (2010), which held that the Second Amendment applies to the states through the Fourteenth Amendment’s Due Process Clause.
This ruling affirmed the individual right to bear arms as a fundamental right protected from infringement by both federal and state governments.
Arguments for and Against Applying the Second Amendment in the Context of Pandemic-Related Gun Store Closures
The recent appeals court decision raises complex questions about the balance between public health measures and the Second Amendment. Arguments for applying the Second Amendment in this context center on the fundamental right of individuals to self-defense, particularly in times of heightened uncertainty and potential civil unrest.
Proponents argue that gun ownership is essential for personal security and that restricting access to firearms during a pandemic infringes on this fundamental right.Conversely, opponents argue that the government has a legitimate interest in protecting public health and safety, and that temporary restrictions on gun store operations are necessary to mitigate the spread of disease.
They contend that the Second Amendment does not guarantee an unfettered right to acquire firearms at all times, and that public health emergencies warrant reasonable limitations on access.
The Second Amendment, like other constitutional rights, is not absolute.
This case highlights the ongoing tension between individual rights and public safety, particularly in the context of evolving public health challenges. The courts will continue to grapple with the application of the Second Amendment in a variety of contexts, including emergencies and other situations where public safety concerns intersect with the right to bear arms.
Final Summary
This ruling has far-reaching implications for future pandemic-related restrictions on businesses and the delicate balance between public health and individual liberties. It underscores the importance of carefully considering the potential impact of restrictions on constitutional rights and ensuring that they are narrowly tailored to address the specific public health threat.
The debate surrounding this case highlights the complexities of navigating a crisis while safeguarding fundamental freedoms, and it’s a debate that is likely to continue as we face future challenges.
The recent federal appeals court ruling that two California counties violated constitutional rights by shutting down gun stores during the pandemic is a reminder that even in times of crisis, individual liberties must be protected. This case highlights the importance of striking a balance between public safety and individual freedoms.
It also brings to mind the recent revelations about the silent killer inside China’s military balloon program , which underscores the need for vigilance in safeguarding our nation’s security. The gun store ruling is a significant victory for Second Amendment rights and a testament to the power of the courts to ensure that government actions are consistent with the Constitution.
The federal appeals court ruling on California counties’ pandemic gun store shutdowns raises interesting questions about the balance of public health measures and individual rights. It’s a complex issue, especially when considering recent studies like this one boosted people more likely than unvaccinated to be infected study which highlight the evolving nature of the virus and the effectiveness of vaccines.
The court’s decision underscores the importance of careful consideration of these factors when implementing public health restrictions.
It’s been a wild ride navigating the legal landscape of pandemic restrictions, and the recent federal appeals court ruling on gun store shutdowns in California is just another example. It’s a reminder that our rights are not always easily protected, even in times of crisis.
While the court recognized the importance of public safety, it also acknowledged the need to balance that with individual freedoms. It’s a delicate dance, and it’s worth noting that experts are sounding the alarm about the potential dangers of platforms like TikTok, which they believe could be used as an intelligence weapon by the CCP.
tiktok a ccp intelligence weapon experts sound alarm on threat The gun store ruling is a good example of how our rights can be challenged, and the potential threat of platforms like TikTok shows that we need to be vigilant about protecting our freedoms in all aspects of life.